Peripheral Artery Disease Treatment Cost in India
Unlock Exclusive Discount : Your Gateway to Premium Healthcare with Medsurge India Health Value Card.

Unlock Exclusive Discount : Your Gateway to Premium Healthcare with Medsurge India Health Value Card.

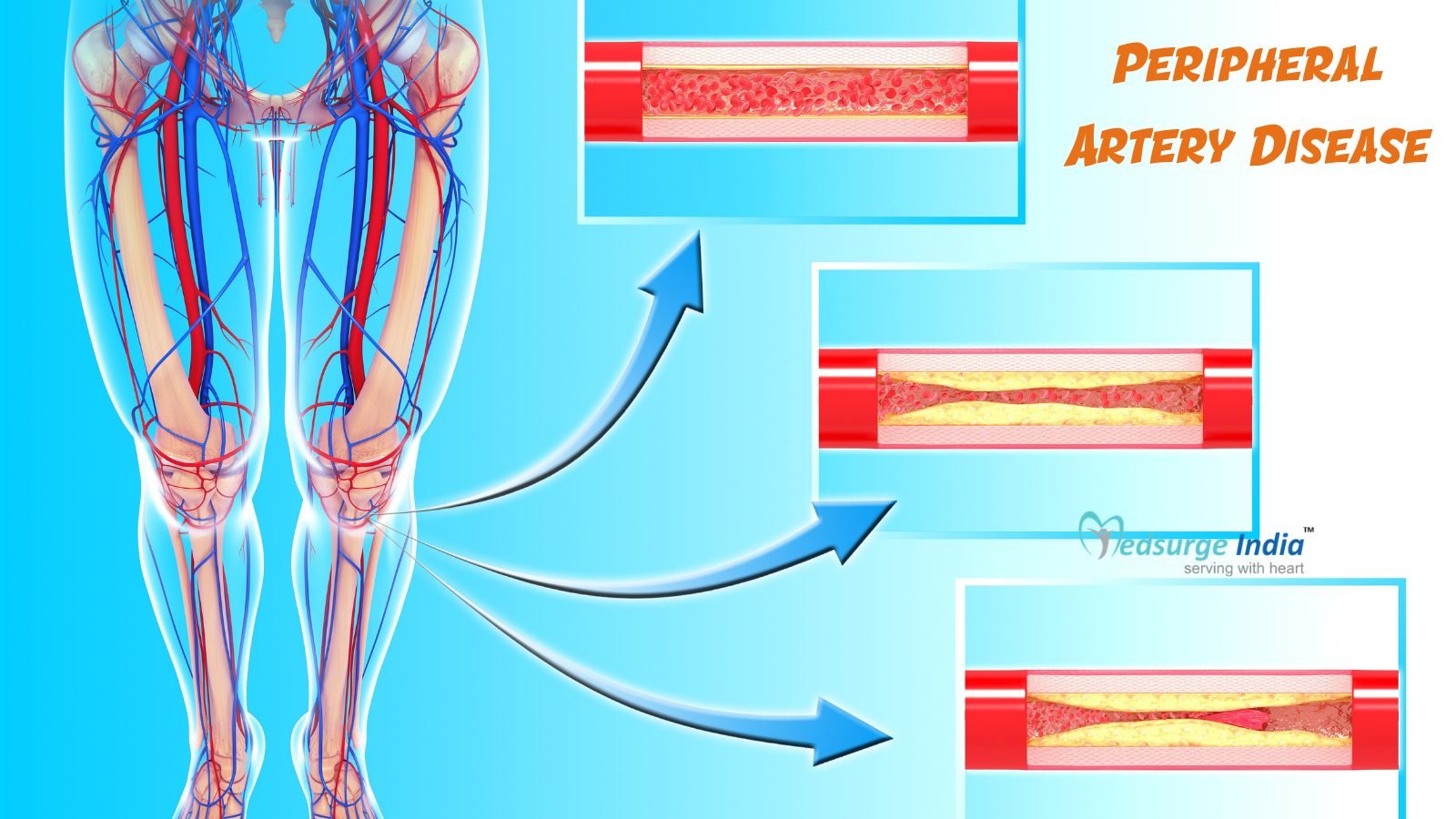
Diseases of the blood vessels beyond the heart and brain are referred to as peripheral artery disease (PAD). An accumulation of fatty deposits in the arteries is the most common cause. Peripheral arterial disease (PAD) is also known as a peripheral vascular disease (PVD) (which includes both arteries and veins).
PAD damages blood arteries, narrowing them and reducing blood flow to the arms, kidneys, stomach, and, most commonly, the legs.
Physical activity can significantly improve symptoms, despite the fact that the disease can have dangerous implications.
Plaque buildup in the leg arteries that deliver oxygen and nutrient-rich blood from your heart to your arms and legs is known as a peripheral arterial disease (PAD), also known as peripheral vascular disease or peripheral artery disease.
A smooth lining avoids blood clotting and facilitates steady blood flow in arteries, which are shaped like hollow tubes. Plaque (composed of fat, cholesterol, and other substances) that accumulates gradually inside your arterial walls narrows your arteries when you have peripheral artery disease. Atherosclerosis is another name for this plaque.
The exterior of many plaque deposits is hard, while the inner is soft. Platelets (disc-shaped particles in your blood that help it clot) can come to the place where the hard surface cracks or tears, allowing them to clot. Blood clots can form around the plaque, narrowing the artery.
Blood can not get through to supply organs and other tissues if arteries become restricted or clogged by plaque or a blood clot. The tissues below the blockage suffer damage and finally die (gangrene). Your toes and feet are the most common places where this happens.
The rate at which PAD advances differs from individual to individual and is determined by a variety of factors, including the location of the plaque in your body and your overall health.
The average cost of Peripheral Artery Disease Treatment in India can range from between 1200 USD to 3000 USD. It typically includes necessary preoperative tests, and the surgery itself. However, please note that accommodation and transfers are not included in this cost.
| Treatment | Starting Price |
| Peripheral Angioplasty | USD 1330 |
| Balloon Angioplasty | USD 2130 |
| Arterial Aneurysms | USD 4370 |
Note: Keep in mind that the aforementioned cost provided is solely for the treatment. The overall cost of Peripheral Artery Disease Treatment in India will be determined based on several factors.
Various factors can affect the cost of Peripheral Artery Disease Treatment in India. Your budget is greatly impacted by numerous elements that fail under pre and post-treatment costs. Below are the various factors that can affect the cost of Peripheral Artery Disease Treatment in India.
Peripheral Artery Disease Treatment Cost in India offers exceptional medical services and facilities to patients who come for treatment in India also their facilities rival those of well-known healthcare centers worldwide. Accommodation, meals, and transportation expenses are also covered. Furthermore, a foreign patient can save up to 30-40% of the Peripheral Artery Disease Treatment cost in India when compared to their native countries.
Many patients with peripheral artery disease have mild or no symptoms, although other people have leg pain when walking (claudication).
Claudication causes muscle soreness or cramping in your legs or arms that is induced by activity, such as walking but goes away after a few minutes of rest. The position of the clogged or narrowed artery determines the location of the pain. The most prevalent site of pain is the calf.
Claudication can range in severity from slight discomfort to immobilizing pain. You may find it difficult to walk or engage in other forms of physical activity if you have severe claudication.
The following are symptoms of peripheral artery disease:
Diagnosis of Peripheral Artery Disease can be done in a variety of methods, but if the disease is suspected, the doctor will first examine the patient’s legs.
The following are some of the tests your doctor may use to diagnose peripheral artery disease:
Peripheral Artery Disease that goes undiagnosed or untreated can lead to painful symptoms, loss of a limb, an increased risk of coronary artery disease, and carotid atherosclerosis (a narrowing of the arteries that supply blood to the brain).
Because persons with Peripheralartery disease have a higher risk of heart attack and stroke, experts advise people at risk to talk to their doctor about it so that it can be diagnosed and treated early.
Peripheral artery disease treatment has two major goals:
You might be able to achieve these goals by making lifestyle modifications, especially if you are dealing with peripheral artery disease early on. Quitting smoking is the single most essential thing you can do to lower your risk of problems if you smoke. Walking or practising other forms of exercise on a regular basis, as part of supervised exercise instruction, can significantly improve your symptoms.
You will almost certainly require extra medical care if you have signs or symptoms of peripheral artery disease. Preventing blood clots, lowering blood pressure and cholesterol, and controlling pain and other symptoms are all things your doctor may recommend.
In some circumstances, angioplasty or surgery may be required to treat claudication caused by peripheral arterial disease. Other prefered surgeries done to cure PAD are the following:
To improve the distance you can walk painlessly, your doctor will most likely suggest a supervised exercise training programme. Regular activity helps your body use oxygen more efficiently, which improves Peripheral artery disease symptoms in a variety of ways.
Peripheral Artery Disease raises the risk of heart attack and stroke, therefore it's critical to get it identified very away. Perspective is influenced by a variety of factors, however, following the lifestyle recommendations above can considerably improve your outlook.
Some cases of Peripheral artery disease can be treated with just a change in lifestyle and medicines.
A: If left undiagnosed and untreated, one in every five patients with PAD will have a heart attack, stroke, or die within five years. In addition to leg muscle pain, discomfort during activity, and loss of mobility and independence, untreated PAD can have other serious consequences.
A: This disease is life-threatening and can lead to death. Lower-body peripheral artery disease is frequently a warning indicator. Other arteries, such as those that supply the heart or the brain, can accumulate plaque in a similar way.
A:
A: Your blood can now flow freely where it is needed, bypassing the barrier. You will not be awake for this surgery, which takes 2 to 5 hours. Typically, you will spend 3 to 7 days in the hospital.
A: The average recovery period for angioplasty is two weeks, however, this can vary depending on your health. Stick to Your Medication Regimen: It's critical to follow your medication schedule. Stopping your medicine too soon can put you at risk for a recurrence of cardiac condition.

Vascular Surgeon
Senior Consultant
14+ years of experience
Narayana Multispeciality Hospital, Rakhial, Ahmedabad
View Doctor
Vascular Surgeon
Associate Consultant
13 years of experience
Medanta – The Medicity, Gurgaon
View Doctor
Vascular Surgeon
Consultant
12 years of experience
M.S. Ramaiah Medical Teaching Hospital, Bangalore
View Doctor
Vascular Surgeon
Senior Consultant
12 years of experience
Max Super Speciality Hospital, Patparganj, New Delhi
View Doctor
Vascular Surgeon
Consultant
22 years of experience
Saifee Hospital, Mumbai
View Doctor
Vascular Surgeon
Consultant
17 years of experience
Manipal Hospital (Old Airport Road) Bangalore
View Doctor
Vascular Surgeon
Senior Consultant
15 years of experience
University College of Medical Sciences, New Delhi
View Doctor
Vascular Surgeon
Director
25 years of experience
Care Hospitals, Banjara Hills, Hyderabad
View Doctor
Vascular Surgeon
Consultant
14 years of experience
Manipal Hospital (Old Airport Road) Bangalore
View Doctor
Vascular Surgeon
Consultant
21 years of experience
Prashanth Multi Speciality Hospital Chennai
View Doctor









By using our site, you agree to our Terms and Conditions, Privacy Policy and Refund Policy. Medsurge India provides reliable healthcare information and treatment options to support informed decision-making. Our content is designed to support and complement the guidance of your treating doctor, helping you feel informed and confident throughout your healthcare journey. We also Accept International Payments.

Copyright © 2025 NSM ONLINE SOLUTIONS PRIVATE LIMITED. All rights reserved.

